 
The T-wave findings in these patients are typically shallow inversions in the inferior leads. 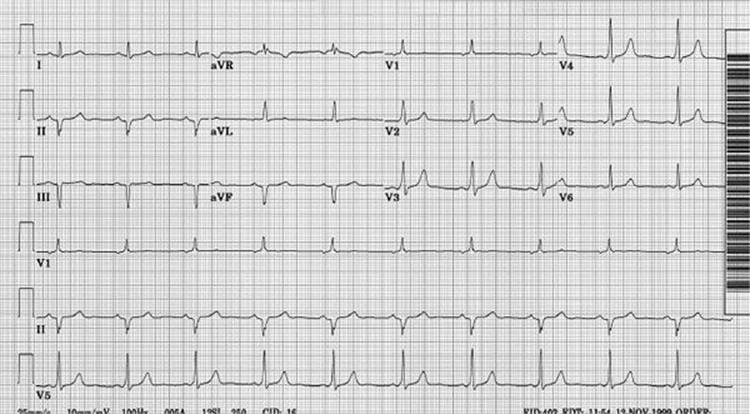
Patients with pulmonary embolism (PE) may also display T-wave abnormalities, including T-wave inversions (Figure 2A). Lastly, patients with past MI can demonstrate persistent T-wave inversions as a manifestation of the MI. In patients with this history and these ECG findings, Wellen syndrome is diagnosed, which is frequently associated with proximal left anterior descending coronary artery critical stenosis the natural history of Wellen syndrome is anterior wall ST-segment elevation myocardial infarction. Pulmonary embolism angina (ie, unstable angina) can present with significantly abnormal T-wave inversions-either symmetric, deeply inverted T waves or biphasic T waves in the precordial leads (V1, V2, and V3 in particular). An important subgroup of patients with pre-infarctionįigure 2A. In general, inverted T waves related to acute coronary syndrome are symmetric in shape this symmetry means that the downsloping limb is a mirror image of the upsloping limb. T-wave inversions associated with coronary artery disease may result from myocardial ischemia (ie, unstable angina), non–ST-segment elevation acute myocardial infarction (NSTEMI-MI), or previous MI (Figure 1A-D). Wellens syndrome (biphasic T wave) Coronary artery disease (acute coronary syndrome, chronic ischemic syndromes) Secondary T-wave changes result from aberrant ventricular activation in the context of normal action potential characteristics examples include bundle-branch blocks, ventricular pre-excitation states (eg, Wolff-Parkinson-White syndrome), ventricular paced rhythms, and ventricular ectopic beats.įigure 1D. Alterations in the duration or morphology of the action potential, without concurrent changes in the orderly sequence of activation, are termed “primary changes.” Primary T-wave inversions are associated with benign syndromes, such as the persistent juvenile T-wave pattern and the digitalis effect, as well as morbid conditions, including acute coronary ischemic events and CNS catastrophe. The causes of T-wave inversions have commonly been grouped into 2 categories: primary T-wave changes and secondary T-wave changes. Wellens syndrome (deeply inverted T wave) Electrophysiologic considerations: primary and secondary T-wave inversion Figure 1C. For example, the patient with an isolated T-wave inversion in lead III in the setting of a musculoskeletal chest pain syndrome would be considered a normal variant ECG finding. This interpretation strategy allows the clinician to discern among normal, potentially abnormal, and abnormal. 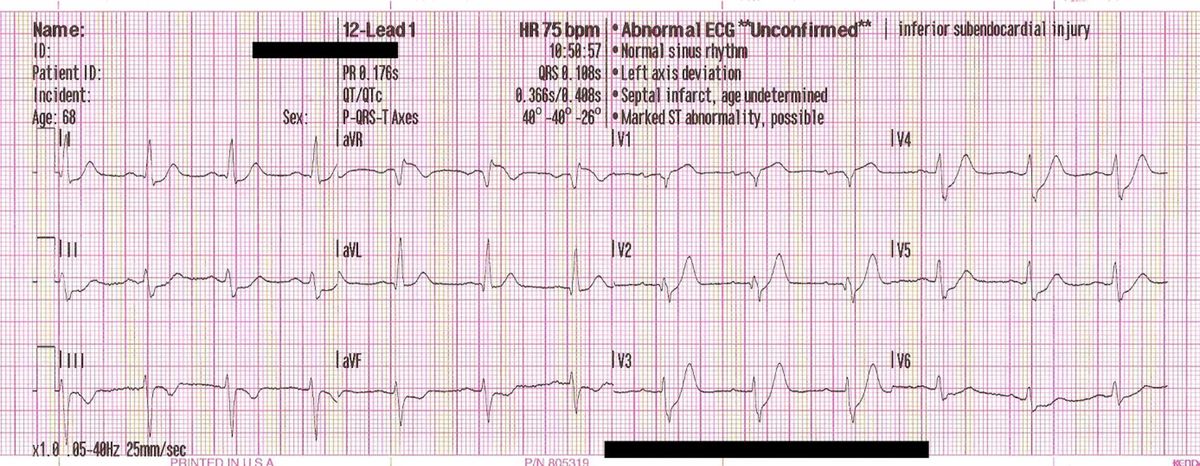
The interpretation of the ECG in the context of the individual patient presentation is mandatory. Acute coronary syndromewave in either lead III or aVF can be a normal variant. In general, an inverted T wave in a single lead in one anatomic segment (ie, inferior, lateral, or anterior) is unlikely to represent acute pathology for instance, a single inverted Tįigure 1B. The T wave is normally upright in leads I, II, and V2 to V6 inverted in lead aVR and variable in leads III, aVL, aVF, and V1. This relative asymmetry may vary because many females and elderly individuals, without identifiable cardiac disease, may have symmetric T waves. The normal T wave has been described to have a gradual upstroke with a more rapid downstroke in the terminal portion. A variety of clinical syndromes can cause T-wave inversions, ranging from life-threatening events, such as acute coronary ischemia, pulmonary embolism, and CNS injury, to entirely benign conditions, such as normal variant T- wave inversions and the persistent juvenile T-wave inversion. Acute coronary syndromecardiac or respiratory syndromes. The natural history of the inverted T wave is variable, ranging from a normal life without pathologic issues to sudden death related toįigure 1A. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
